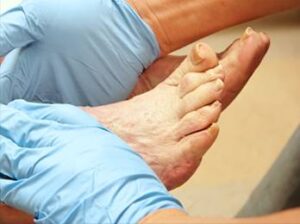
 Unfortunately, foot problems are often a common result of having diabetes. As time goes by, it’s likely that diabetes will cause certain risk factors such as nerve damage, also known as diabetic neuropathy and arterial damage, also known as peripheral vascular disease or PAD. Diabetic neuropathy can lead to tingling or a painful sensation, and it may also cause you to lose feeling in your feet. The loss of feeling in your feet can become incredibly dangerous, especially if you can longer sense a blister or cut on your foot; this can lead to sores or limb threatening infections. Peripheral vascular disease (PAD), also incredibly dangerous, can lead to infection, non healing and tissue loss called gangrene or critical limb ischemia.
Unfortunately, foot problems are often a common result of having diabetes. As time goes by, it’s likely that diabetes will cause certain risk factors such as nerve damage, also known as diabetic neuropathy and arterial damage, also known as peripheral vascular disease or PAD. Diabetic neuropathy can lead to tingling or a painful sensation, and it may also cause you to lose feeling in your feet. The loss of feeling in your feet can become incredibly dangerous, especially if you can longer sense a blister or cut on your foot; this can lead to sores or limb threatening infections. Peripheral vascular disease (PAD), also incredibly dangerous, can lead to infection, non healing and tissue loss called gangrene or critical limb ischemia.
The most common way for a Podiatrist to manage the Diabetic foot is through preventative measures by examination of the skin, sensation of the feet and circulation on a consistent basis. The regular care of thick toenails and callouses in the office is also a common way to manage the Diabetic foot. This simple task can prove greatly beneficial. Modifying Diabetic shoes and insoles are also ways we reduce friction and pressure to areas of concern. As your Podiatrist we inspect the appearance of your feet to note changes that have occurred in between visits. Regular visits may consist of every month, every two months, every 6 months or once a year depending upon each patients risk factors. If a serious condition presents itself, our expert doctors are available to manage the condition in a hospital setting.
There are many ways to maintain healthy Diabetic feet at home. Most importantly, you want to ensure that you’re managing your blood sugars. You also want to ensure that you’re checking your feet daily. As mentioned before, it’s important to recognize if your feet have cuts, sores, blisters, plantar warts, ingrown toenails, or other troubling foot conditions to stay ahead of the issue and prevent yourself from further harm. Along with foot checks, wash your feet daily and apply foot cream daily, avoiding the areas between your toes. It is beneficial to wear diabetic socks, refrain from walking barefoot and avoid smoking. If you do happen to develop a corn or callus, never treat them yourself: seek the help of a podiatrist. If you notice a cut, blister, or bruise is not healing after a few days or redness, swelling, odor, a callus with dried blood inside of it, or an infection that causes discoloration of the foot it is important to seek the help of a podiatrist.
If you’d like more information on how to maintain healthy feet while living with diabetes, seek the assistance of a podiatrist and call our office to schedule an appointment to provide you with the tips needed for healthy foot care.



